Malaria is a vector-borne disease that is responsible for thousands of deaths, most people die due to lack of access to quality health, in this article, we will be looking into the most effective natural home remedies that anyone could apply in an emergency, or when the medical care is not easily accessible.
Warning, this should never replace professional medical advice.
Statistics of malaria
Appropriately half of the world’s population is at risk for developing malaria—most in the lower-income countries of the world. This disease is transmitted in 108 countries of the world in which 3 billion people live, and infects up to 250 million, and kills nearly 800,000 people per year. According to the World Health Organization (WHO), a child dies every 45 seconds as a result of the disease. Malaria exists in parts of Africa, Asia, the Middle East, Central/South America, Hispaniola, and Oceania 350-500 million people each year are diagnosed with Malaria. Over 1 million people die from malaria each year. Most malaria deaths occur in sub-Saharan Africa. Most people who die of malaria are children Malaria was the 4th cause of childhood death in developing countries in 2002 10.7% of childhood.
Susceptible Species for Malaria
About 65 Plasmodium sp. have been isolated from over 1,000 different species of birds. Few of the Plasmodium sp. which has been identified appear to be natural parasites of domestic poultry. A number of other species of Plasmodia that occur primarily in passerine birds can infect or have been experimentally transmitted to the domestic fowl.
Susceptible Host for Malaria
Plasmodium can be pathogenic to penguins, domestic poultry, ducks, canaries, falcons, and pigeons, but is most commonly carried asymptomatically by passerine birds. Humans, reptiles, and other mammals, and non-human primates.
Age Susceptible To Malaria Attack
Research has shown that the age most susceptible to malaria attack is the teenagers, that does not mean that adult do not get malaria, just that the majority of cases (65%) occur in children under 15 years old.
Sex Susceptible To Malaria Attack
Pregnant women are also especially vulnerable: about 125 million pregnant women are at risk of infection each year. According to CDC, this startling statistics in pregnant women is due to the change in women\’s immunity during pregnancy and also the presence of the new organ (the placenta) with new places for parasites to bind, pregnant women lose some of their immunity to malaria infection.
What is Malaria Caused By
There are four types of parasites that are introduced into the bloodstream by the anopheles mosquito. If the disease becomes chronic (recurrent), it results in general debility, anemia, and an enlarged spleen.Severe cases can be very debilitating. An especially deadly form is called blackwater fever. The skin takes on a yellow tint and the urine becomes progressively darker in color. Few people survive three attacks of black water fever. Plasmodium is transmitted between people by blood-eating mosquitoes. The mosquito is described as malaria ‘vector’ because it spreads but doesn’t actually cause disease. To beat malaria, the immune system needs to be able to find Plasmodium.
But Plasmodium hides, first in liver cells and then in red blood cells.This prevents the immune system’s white blood cells from finding and destroying it. Plasmodium has a complex life cycle involving the infection and destruction of red blood cells.Five species of the single-celled protozoan parasite Plasmodium can cause malaria in humans: P. falciparum, P. vivax, P. ovale, P. knowlesi and P. malariae. Of these, P. falciparum, the dominant species in Africa, is the deadliest and is responsible for approximately 90% of malaria deaths per year. However, it has been estimated that more people worldwide live at risk from P. vivax than P. falciparum and as a result suffer increased morbidity from P. vivax.
Each species of the Plasmodium parasite differs in phenotype, immune response, geographical distribution, relapse pattern, and drug response. Malaria is a vector borne disease transmitted from one person to another by certain species of blood-sucking mosquitoes of the Anopheles genus which includes: A. gambiae – the primary vector for transmission of P. falciparum malaria in sub-Saharan Africa. Female mosquitoes transmit malaria as they feed on blood; they need high levels of proteins in the blood meal to develop their eggs.
They are attracted to humans by smell and vision. Slender, sharp, saw-toothed stylets on the end of the female mosquito’s proboscis pierce the skin and probe for a suitable small blood vessel. While sucking up the blood, the mosquito pumps saliva into the host. Chemicals in the saliva prevent the blood from clotting and act asan anesthetic to stop the host from feeling the mosquito while it is feeding. The characteristic red, itchy swelling of a mosquito bite is due to an allergic reaction to the leftover saliva. Male mosquitoes do not transmit the disease as they feed only on plant juices.
Life Cycle of Malaria
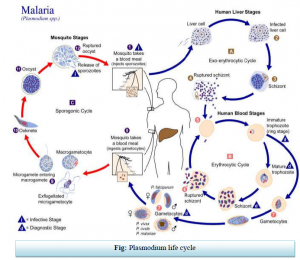
The Plasmodium parasite has a complex life cycle characterized by alternating extracellular and intracellular forms, involving sexual reproduction in the mosquito and asexual reproduction in the liver cells and RBCs of humans (see diagram). The parasite enters the human host when an infected mosquito takes a blood meal.
Sporozoites from the mosquito’s salivary glands are injected into the host’s bloodstream. Within 30 minutes the sporozoites will have entered the host’s liver cells. The sporozoites feed on the cell contents, grow and change to form schizonts. Over the next 5–8 days they divide rapidly, forming thousands of merozoites. The liver cells balloon and burst[5], releasing merozoites into the bloodstream where they invade the RBCs. While the parasite is within the liver, the person does not feel sick and shows no signs or symptoms of the disease. P. vivax and P. ovale can have a dormant stage in the liver called hypnozoites. Thesecan remain in the liver for several years, causing relapses in later life.
While in the liver and the RBCs the parasite is protected from the host’s antibodies. Inside the RBCs the individual merozoites develop into trophozoites and finally into schizonts which contain up to 32 distinct merozoites, depending upon the species of Plasmodium. After 2–3 days the RBCs rupture, releasing the merozoites back into the bloodstream. These merozoites go on to invadeuninfected RBCs and the cycle continues.
As the RBC ruptures toxins are released from the merozoites.It is believed that these toxins directly stimulate the host’s immune system and a highly complex immune response is initiated, resulting in bouts of chills, fever, and sweats. In P. vivax malaria this can occur once every 48 hours, corresponding to the RBC cycle. Some of the trophozoites develop into male and female gametocytes, the sexual stages of the parasite.
These circulate in the blood and aretaken up by the female mosquito when it takes a blood meal. Inside the mosquito’s stomach, the gametocytes develop into gametes, fertilizationoccurs and a zygote is formed. Within 24 hours the zygotes transform into motile ookinetes thatburrow into the stomach wall. Ookinetes encyst and become oocysts that divide to produce approximately 1,000 sporozoites each. After about 7 days the oocysts rupture, releasing their sporozoites, which make their way to the salivary glands ready to infect another human.
Malaria Symptoms and Signs
Chills occur for several hours, followed by drenching sweats every 1-3 days, the signs of malaria may be seen in a person’s complexion.
How Malaria is Prevented
Removing or poisoning the breeding grounds of the mosquitoes or the aquatic habitats of the larva stages, by applying oil on standing water or destroying or discarding any container that can hold water. Indoor residual spraying (IRS) is the practice of spraying insecticides on the interior walls of homes in malaria-affected areas. Mosquito nets help keep mosquitoes away from people, and thus greatly reduce the infection and transmission of malaria. The nets are not a perfect barrier, so they are often treated with an insecticide designed to kill the mosquito before it has time to search for a way past the net.
Home remedies for malaria
Quinine for Malaria

USE OF QUININE:It is a bitter-tasting drug made from cinchona bark used for the treatment of malaria. Quinine will generally eliminate malaria, but ulcers and pains in the bones, loss of teeth, loss of memory, and impaired sight, a mild to severe hearing loss may also result. Quinine is used internally to correct loss of appetite, dyspepsia, and flatulence with a sense of fullness. The bark is used for malaria, flu, enlarged spleen, muscle cramps, muscle pain, cancer, and gastric disorders. Externally, it is used for scrapes and skin ulcers. Chinese Medicine: Quinine is used for malaria, fever and alcohol intoxication. The drug is used to treat intermittent fever, malaria, intercostal neuralgia, sciatica, and neuritis (especially of the arm), in India. Homeopathic Uses: Quinine is used to treat general poisoning, attacks of fever, inflammation of the respiratory tract, acute diarrhea, anemia, general debility, skin rashes, and neuralgia.
CONTRAINDICATIONS Quinine should not be used during pregnancy.
PRECAUTIONS AND ADVERSE REACTIONS: General: Sensitization to Quinine and Quinidine has been observed (eczema, itching). Even at therapeutic dosages, an enhanced pseudo hemophiliac effect can occur through the triggering of thrombocytopenia. Drug Interactions: Because of the possibility of thrombocytopenia, care must be taken when Quinine preparations are administered along with other drugs that are known to precipitate thrombocytopenia.
OVERDOSAGE: In cases of overdose (more than 3 gm Quinine) or of long-term administration of the drug or its alkaloids, nausea, summer cholera, headache, fall of body temperature, intravascular hemolysis, cardiac arrhythmias, buzzing in the ears, hearing and visual disorders (all the way to complete deafness and blindness) may occur. Death comes with dosages of 10 to 15 gm of Quinine through heart failure and asphyxiation. Following gastric lavage, the symptomatic therapy for acute poisonings includes atropine for bradycardia and phenytoin in the presence of tachycardic heart rhythm disorders. Forced diuresis and hemodialysis are not suitable as therapeutic measures.
DOSAGE Mode of Administration: Whole, cut and powdered drugs is used in various galenic preparations, including tonics, drops, tablets, compresses, ampules, coated tablets, suppositories and compound preparations. Preparation: A tea is prepared by pouring 150 ml of boiling water over 1/2 teaspoonful of the drug and allowing it to draw for 10 minutes. A decoction is prepared by adding 0.5 g to 1 teacup of water. A tincture in the proportion of 1:5 in 75% ethanol is also used.
Daily Dosage: Total daily dose is 1 to 3 gm of the drug. The liquid extract daily dose is 0.6 to 3 gm of cinchona liquid extract, which contains 4 to 5% total alkaloids. A daily dose of 0.15 to 0.6 g cinchona extract with 15 to 20% total alkaloids may also be used. The standard single dose of the extract is 0.2 gm. The liquid extract single dose is 0.5 to 1 gm. Homeopathic Dosage: 5 drops, 1 tablet or 10 globules, every 30 to 60 minutes (acute) or 1 to 3 times a day (chronic); parenterally: 1 to 2 ml Sc, acute: 3 times daily; chronic: once a day (HAB1). Storage: Keep protected from light and moisture.
INFLAMMATION AND BLOODY BOWELS FROM MALARIAL FEVER: [CHARCOAL WATER AND POULTICES]
Charcoal for Malaria Fever.

Pulverized wood charcoal. An inert substance but with healing potential. Has the power to neutralize putrid smells of cancer, diarrhea, gangrene, and a great capacity for absorbing gases. Its latent power is brought to life by prolonged trituration (grinding finely and diluting) with sugar of milk. To counter the effects of dangerous drugs. In the absence of sterile dressings and modern hospital amenities, powdered vegetable charcoal has an ancient reputation as an astringent dressing. It absorbs bacterial toxins and is useful for chronic bowel discharge.
Powdered charcoal dressings were used during World War I. Rubbed in lard, was used for purulent foul discharging wounds to neutralize the smell and promote healing. Other indications: relaxed veins, stomach tense and full of wind, constant belching. For weak and cachectic individuals where, vital powers are weak. Available in biscuits, tablets, and capsules for its purifying properties and as an aid to digestion. Tablets containing a high sodium content should be avoided. Powdered charcoal will help purify the blood.
How To Use NEEM OIL OR HERB For Malaria

No health hazards or \”side effects are known in conjunction with the proper administration of designated therapeutic dosages. Recent research This indicates that Neem oil is both anti-inflammatoryand antibacterial, and to some degree reduces fever and lowers blood sugar levels. Insecticide Extensive research shows that liminoid azadirachtins areinsecticidal and inhibit feeding and growth—making Neem an inexpensiveand ecologically sound insecticidal agent. The azadirachtins are also linked to the tree’s antimalarial activity.
Diabetes Research indicates that neem leaf and oil act to stabilize blood sugar levels and may be helpful in treating or delaying type 2 diabetes. Traditional & Current Uses Medicine chest Thought of in India is almost a pharmacy in its own right, all parts of the neem tree may be used medicinally. The bark is bitter and astringent, and a decoction is used for hemorrhoids. The leaves are taken as an infusion for malaria, peptic ulcers, and intestinal worms, and maybe applied locally as a juice, infusion, or ointment to skin problems including ulcers, wounds, boils, and eczema.
The juice of the leaves is also applied to the eyes to treat night blindness and conjunctivitis. The twigs are used as a tooth cleanser, firmingup the gums and preventing gum disease.
DOSAGEMode of Administration: The drug is available as a tincture. A slightly narcotic decoction can be prepared (said to lower a fever). An ointment for killing lice is administered topically.
LEMON JUICES for Malaria

Lemon is used as a source of vitamin C in cases of general low resistance, scurvy, and colds. In folk medicine, lemon juice was recommended as a drink for fever, as a remedy for acute rheumatism and as an antidote to intoxicants, particularly opium. Additional traditional uses that are still recommended include sunburn and as a quinine substitute for malaria or to reduce body temperature in” typhus patients. Indian Medicine: Uses in Indian medicine include as a remedy for shaking and heartburn.
WORMWOOD For Malaria

Bitter herb Research into wormwood, mostly during the 1970s, has established that a range of the constituents within the plant contributes to its medicinal activity. Many are very bitter, affecting the bitter taste receptors on the tongue which sets off a reflex action, stimulating stomach and other digestive secretions.
Gut inflammation; A German clinical trial in 2007 found thatwormwood helped in treating Crohn’s disease (an inflammatorybowel disorder). Wormwood prevented the return of symptoms in90% of those taking it, and reduced the required dosage of powerful steroiddrugs are taken to control inflammation. Patients also experienced lower levels of depression. Other research Constituents within wormwood, notably the essential oil, are thought to have wide-ranging therapeutic effects, including neuroprotective, antidepressant, antibacterial, antifungal, and antimalarial activity. Wormwood is commercially available as an essential oil, as well as in capsule, tablet, tincture, and aqueous extract dosage forms.
Goldenseal tea for Malaria

DOSAGEDaily Dosage:Extract — Standardized extract (5% hydrastine) 250-500 mg 3 times daily (Werbach & Murray, 1994). Fluid extract — lU to 1 teaspoonful (1.25-5 ml) (Grieve, 1971) Solid extract — 325-520 mg (Grieve, 1971), Local antiseptic — 1 teaspoonful powder steeped in 1 cup boiling water for 15 minutes. Swish around the mouth or gargle for mouth or throat sores (Tyler, 1997). Travelers diarrhea — One capsule (500-1000 mg root) 3times daily (Tyler, 1997).
MILK THISTLE for Malaria

Herbal Use: Traditionally, milk thistle fruits have been used for disorders of the liver, spleen, and gall bladder such as jaundice and gall bladder colic. Milk thistle has also been used for nursing mothers for stimulating milk production, as a bitter tonic, for hemorrhoids, for dyspeptic complaints, and as a demulcent in catarrh and pleurisy. It is stated to possess hepatoprotective, antioxidant and choleretic properties.
Current interest is focused on the hepatoprotective activity of milk thistle and its use in the prophylaxis and treatment of liver damage and disease. The leaves have also been used for the treatment of the liver, spleen and gall bladder disorders and as an antimalarial, emmenagogue and for uterine complaints. Milk thistle leaf preparations are available today, although most research has been conducted with preparations of the fruit since the leaf does not contain the pharmacologically active component silymarin.
Dosage: Dosages for oral administration (adults) for traditional uses recommended in standard herbal reference texts are given below. Fruit Crude drug 12–15 g daily in divided doses (equivalent to silymarin 200–400 mg daily). (G3) Herb Approximately 1.5 g of finely chopped material as a tea, two or three cups daily. The doses of silymarin used in clinical trials have ranged from 280–800 mg/day (equivalent to milk thistle extract 400–1140 mg/day standardized to contain 70% silibinin). (3) For hepatic disorders, doses of up to 140 mg (equivalent to 60 mg silibinin) two or three times daily have been suggested. (G43) In Germany, the recommended regimen for treatment of Amanita phalloides poisoning with a standardized silymarin preparation (Legalon) is a total dose of silibinin (as the disodium hemisuccinate) (20 mg/kg body weight) over 24 hours, divided into four intravenous infusions each given over a 2-hour period
LEMON-GRASS for Malaria Treatment

In rats, i.v. administration of an infusion caused a drop in arterial pressure and a mild diuretic effect. The oral administration of an imprecise amount of extract caused a drop in temperature and a tendency to lengthen intestinal passage. Because of the small number of experiments carried out, a hypotensive action cannot be considered as conclusively proven. The essential oil has an antibacterial effect in animal tests: in higher doses, it has a sedative/ analgesic effect.
INDICATIONS AND USAGE: Unproven Uses: Externally, Lemongrass is used for lumbago, neuralgic and rheumatic pain, sprains, and as a mild astringent. Internally, the herb is used for gastrointestinal symptoms and mild states of agitation. Indian Medicine: Lemongrass is used for intestinal parasites, stomach complaints, flatulence, leprosy, bronchitis and fever.
STEAM BATH for Malaria
Have a steam bath ready and hot when the attack is expected, while in the chill give a steam bath before the fever starts. If done properly there is no more malaria unless you get a mosquito bite again. If you are too late with the heat, get it at the next chill. Read the step-by-step guide on HOW TO GIVE STEAM BATH here. If this treatment is rightly done, the malaria parasite will be destroyed, and follow up with a good and healthy diet to build your immune system. I have done this treatment for myself and for many others it works like magic. Please watch your guest or patient with care and give ears to their complains, if the heat much reduces a bit, always change the cold compress towel on the forehead every minute to prevent the heat from causing damage to the brain
References
- Thrash. A. (1981). Home remedies.
- Centers For Disease Control and Prevention-[https://www.cdc.gov/malaria/malaria_worldwide/reduction/iptp.html]
- Thomas Bartram, Bartram’s Encyclopedia of Herbal Medicine
- Sinclair, M. (2008). Modern hydrotherapy for the massage therapist.
- Medline plus, (2011). Vital Signs.
- Dail, C, Thomas. C., (1995). Hydrotherapy: simple treatments for common ailments.
- Malaria, A global challenge.
- Encyclopedia of Herbal Medicine Andrew Chevallier FNIMH
- Harrison’s principles of internal medicine. (18th Ed.).
- British Society for Immunology (Malaria poster).
- Vance. Ferrel. Harold. M, Cherne, MD. Natural-Remedies-Encyclopedia-4th-Edition.
- Herbal Medicines, Third edition-Joanne Barnes J.David Phillipson Linda A. Anderson.
- PDR for Herbal Medicines.